Benign Paroxysmal Positional Vertigo (BPPV)

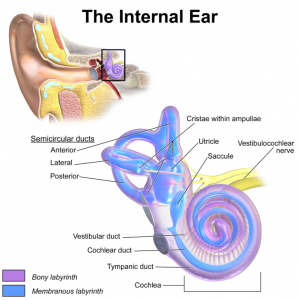
The vestibular system is one of the three systems in our body including the sensory and visual systems that help provide sensory information that allows us to balance. The vestibular system lives within the inner ear and helps determine where our body is in space. One of the components of the vestibular system is the semicircular canals. There are three semicircular canals in each ear which are orientated 90 degrees to each other so that they detect movements in all different planes. Each canal is lined with setereocilia which are very fine little hairs. The canals are then filled with a fluid called endolymph which has a similar viscosity to honey. When the head is moved the endolymph moves and then the hairs that when move fire messaged to the brain and report that movement.
There are also otoliths which are found in the utricle of the vestibular system. Otoliths are made out of calcium carbonate and help detect linear movements of the head.
BPPV is the most common cause of dizziness in adults and different papers report it as the cause of dizziness for between 45-60% of over 80 year olds. BPPV most commonly affects people over the age of 50. BPPV is caused when otoconia (calcium carbonate tiny crystals) find themselves in the semicircular canals and not the utricle. The cause of why this happens goes largely unknown, this is called idiopathic BPPV and is the most common variety. There is also a higher incidence of BPPV when also suffering from head injury, vestibular neuronitis, migraine, osteoporosis and osteopenia, menieres and labrinthitis. Women are also twice as likely to get BPPV than men.
There are two different places that the otoconia can be found within the semicircular canals;
- Floating within the canal: Canalithitis
- Adhered to the cupula at the end of the semicircular canal: Cupulolithiasis
The main differences between the two are that canalithitis is much more common and has a short duration of symptoms (less than 1 minute) in the provocative position whereas with cupulolithiasis symptoms are generally sustained for the duration of the provocative position.
The most common canal to be affected by BPPV is the posterior semicircular canal accounting for 89-90% of cases followed by the Horizontal Semicircular canal accounting for 10-31% and lastly the Anterior Semicircular Canal coming in at 1-20%.
How would I know if I have BPPV?
The key subjective features of BPPV include
- Short episodes of vertigo that are brought on by certain head position and movement such as getting in and out of bed, looking up, rolling in bed.
- Vertigo that feels like the world is spinning around you
Assessment of someone with BPPV
It is first paramount that your health professional rules out some of the other causes of vertigo before continuing treatment. BPPV should not cause problems with coordination of movement, speech or swallow, bowel or bladder problems, sever head pain or pressure, weakness pins and needles or numbness. Please seek immediate medical attention if you are suffering from any of the above problems.
There are some main tests that look at each of the canals
- Dix hallpike: For Anterior SCC and PSCC
- Sidelying test: For Anterior SCC and PSCC. A slightly less intimidating test that the dix hallpike for when clients are very ill, nervous or neck extension is contraindicated
- Supine Roll test: For the anterior SCC
- Bow and lean test: Assists in identifying which side is affected for the Horizontal SCC
What is my physio looking for?
During the positional testing your physio is looking to reproduce your symptoms of vertigo and in particular examine any abnormal eye movement called nystagmus. The direction and rotation of the abnormal eye movement can provide information as to the type of problem driving the dizziness and the side of the body where the problem is. With Posterior canal problems a torsional upbeating nystagmus is present to the side of the lesion, horizontal direction changing nystagmus in the horizontal canal and downbeating torsional nystagmus in the anterior canal.
How can my physio treat my BPPV?
Before treating your physio must first determine which side is affected and whether you have canalithiasis or cupuloithiasis. A Canalith Repositioning Technique (CRT) is used by your physio to drain the otoconia out of the SCC. The most common canalithiasis CRT for the posterior SCC is an Eply manouver or Brandt-Daroff exercises. For the Horizontal canal a BBQ Roll or Gufoni is used and an Eply or Deep head hang for the Anterior SCC. In the instance of cupuloithiasis often speed needs to be used to detach the otoconia from the cupula. A sermont is then the preference for the Posterior canal, a Gufoni or Modified Sermont for the Horizontal Canal and a Modified Sermont for the Anterior canal. These techniques sometimes have to be followed by a canalithiasis CRT to drain the otoconia properly out of the canal. These CRT are generally performed between 1-3 times per session depending on the tolerance of the client.
It is common that the clients symptoms are aggravated during the process of treatment and this can sometimes feel like a bad hangover for 1-2 days. BPPV can often take more than 1 session to clear the otoconia and can sometimes reoccur. There is a 15-20% reoccurrence rate to any given episode and a 50% reoccurrence within 10 years.
Immediately after treatment clients should try and remain upright for 20-30 minutes, sleep with 2 pillows and avoid their previously aggravating head positions and movements for 2-3 days.
If I am a physio how can I learn more about this?
I must firstly honour Natalie Rando and Leia Barnes whose Vestibular course I had the privilege of attending. This blog reflects much of their intelligence not my own. A lot of their blood,sweat and tears have gone into a wonderful course that I learnt an exceptional amount on. You can find them on www.vestibularcourses.com.au
Lindsay Christie (APAM)
Physiotherapist

References
Gold, D. R., Morris, L., Kheradmand, A., & Schubert, M. C. (2014). Repositioning maneuvers for benign paroxysmal positional vertigo. Current treatment options in neurology, 16(8), 1-22.
Hilton, M. P., & Pinder, D. K. (2004). The Epley (canalith repositioning) manoeuvre for benign paroxysmal positional vertigo. The Cochrane Library.
Herdman, S. J., Hall, C. D., Schubert, M. C., Das, V. E., & Tusa, R. J. (2007). Recovery of dynamic visual acuity in bilateral vestibular hypofunction. Archives of Otolaryngology–Head & Neck Surgery, 133(4), 383-389.
Keshner, E. A., Hain, T. C., & Chen, K. J. (1999). Predicting control mechanisms for human head stabilization by altering the passive mechanics. Journal of Vestibular Research, 9(6), 423-434.









When you suffer from vertigo, a hearing impairment is probably not the first thing that comes to mind. But vertigo can be a very serious impairment associated with hearing loss. So you should make an appointment with an audiologist just to be sure, and to rule out this possibility.
Check out this article for some tips: http://www.hearlink.com.au/industry-news/spotlight-vertigo/