Diagnosis: Stress Fracture
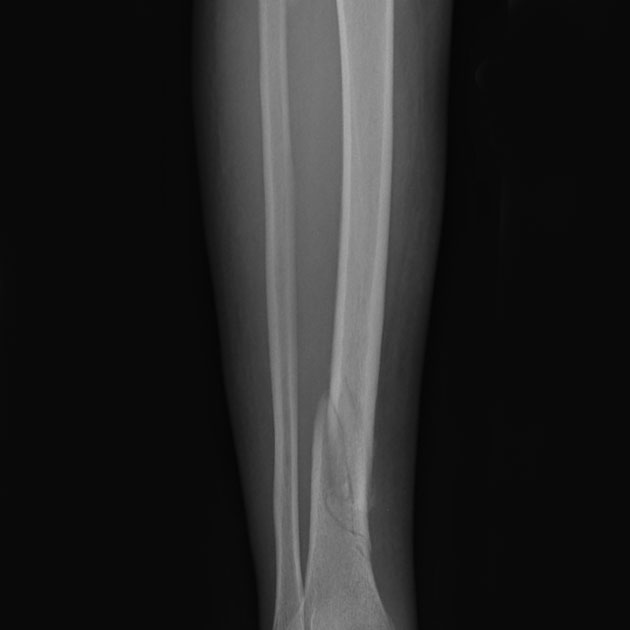
Stress fractures are partial or complete fractures resulting from repetitive and excessive mechanical stress on bone, not from a single traumatic event like other bony fractures. They typically begin as a stress reaction in the bone due to this loading and, if not treated with sufficient rest for the bone to heal, progress into a stress fracture. They are especially common in the lower leg in athletes involved in running or jumping sports. Common bones affected include the metatarsals, the calcaneus, tibia and fibula, and various parts of the femur. They can also occur in the upper limbs in athletes such as throwers and lifters.
How stress fractures present
Usually, there is pain in the region of the fracture, which increases with physical activity and load. Sometimes the surrounding soft tissues may become swollen, especially when the fracture affects tibia, fibula and feet. The patient may have undergone a sudden increase in training load or intensity, and in women they may have had a disruption to their menstrual cycle. Typically, the patient will describe an insidious onset with localised dull aching pain that is worse with activity.
The patient may have undergone a sudden increase in training load or intensity #performbetter @pogophysio Share on XHow stress fractures are diagnosed
Upon examination, the affected area will typically be tender on palpation. Although joint function and movement are usually not affected, if the fracture is near the joint such as in the hip or ankle, the joint movement can be affected.
Imaging is very important in diagnosing this condition. Plain X-rays can be useful because they can pick up a stress fracture, meaning further imaging is rarely necessary. However, they can also be falsely negative, meaning they can miss the fracture. Bone scintigraphy (bone scans) has long been considered to be the best diagnostic method for stress fractures. MRI can also be used.
Causes of stress fractures
Stress fractures are injuries that occur as a result of repeated loading of the bone. They can occur in two ways: excessive loading to a normal bone, called fatigue fractures, or normal loading to a weakened bone, called insufficiency fractures. Repetitive and excessive stress of normal bone without adequate rest is the primary pathology of stress fractures.
Treatment of stress fractures
The treatment of any type of stress fracture is rest. This may include a period of non-weight bearing, although in most cases simple activity modification and weight bearing as tolerated are sufficient. 4–8 weeks of relative rest is recommended for non-complicated stress fractures. This rest is followed by a gradual return activity. Most stress fractures heal with simple conservative management, avoiding the need for surgery.
The treatment of any type of stress fracture is rest. #performbetter @pogophysio Share on XIn areas that are at a high risk for progression to complete fracture, delayed union or non-union, immobilisation indicated to prevent complications. There are other proposed treatments such as ultrasound, electrical stimulation, laser therapy, foot orthoses, the use of leg braces and non-steroidal anti-inflammatory drugs. The evidence surrounding these however is mixed.
Surgical treatment may be indicated for stress fractures in particular areas. This is suggested particularly in femoral tension stress fractures and in complicated fractures of the talus and navicular, fifth metatarsal, tibia and fibula. Surgery could also be an option for athletes in order to return to sport much faster than possible with conservative management.
Sandi Davis
Student Physiotherapist
References
Aweid, B., Aweid, O., Talibi, S., & Porter, K. (2013). Stress fractures. Trauma, 1460408613498067.
Graham, E. M., Burns, J., Hiller, C. E., Nightingale, E. J., & Simic, M. (2015). Management for common lower leg stress fractures in athletes. Physical Therapy Reviews, 20(1), 29-41.
Peris, P. (2003). Stress fractures. Best Practice & Research Clinical Rheumatology, 17(6), 1043-1061.
Philipson, M. R., & Parker, P. J. (2009). Stress fractures. Orthopaedics and Trauma, 23(2), 137-143.








