Blood Flow Restriction Training (BFRT)

It has been believed that to increase muscles size and strength you must lift heavy weights. Modern research into the use of blood flow restriction training has shown that lifting as light at 20% of your maximum effort can result in increases in these measures. So can you really lift light weights and still get big and strong, let’s find out…
What is it?
The idea was originally born in Japan during the 1970’s by a man named Dr. Yoshiaki Sato however it wasn’t popularised outside of Japan until the 2000’s. Sato was the original experimenter of ‘KAATSU training’ which is essentially the same as blood flow restriction training (BFRT) (12).
As the name suggests, the principle is to reduce the blood flow of a limb whilst performing resistance or endurance exercise. This is achieved by placing a pneumatic tourniquet around either the upper thigh or arm. This air-filled cuff occludes venous flow but allows continuation of a reduced arterial inflow. Put simply, blood gets into the limb but can’t escape.
Now, what is the benefit of this you might ask. The amazing thing about BFRT is that strength and muscle hypertrophy gains can still be made but at a MUCH lower exercise intensities. It was always thought if you wanted to gain strength and build muscle that you need to be lifting weights that are >60-70% of your 1 rep maximum (1RM) (1). With BFRT you are able to lift 20-30% 1RM and still make these gains. Normally such light weight would only cause strength and hypertrophy gains when lifted until volitional fatigue.
So BFRT is great for clinical populations who may be recovering from an injury or have a reduced ability to perform exercise due to musculoskeletal weakness (5). Small studies have shown promising results for rehab both following knee arthroscopy (11) and Achilles tendon rupture (13). BFRT is also useful in elderly populations. A 2019 review study found that elderly populations who just walked with BFR had increases to muscle size and strength (3). BFRT is also implemented by advanced strength trainers such as elite athletes and bodybuilders who may require a novel stimulus to force muscle adaptation after years of training (6).

BFRT applied to the upper thigh
How to do it
As the science of BFRT is still in its infancy and a variety of protocols and equipment are used. Therefor there is not a one size fits all answer. Below is a general guideline based on the current literature.
The Cuff
Different studies utilise different occlusion devices ranging from automatic
pneumatic tourniquet systems to handheld manual blood pressure cuffs and newer elastic wraps (9). Cuff width can range from 3-18cm and the wider the cuff, the less pressure that needs to be applied (10).


Cuff types. Left; elastic straps, right; manual cuff, below; automatic cuffs

Pressure Settings
Most studies seem to cite 40-80% of arterial occlusion pressure as a safe range for BFRT. This is simply means 40-80% of the pressure required to stop blood flow to the limb. It has recently been shown that even the lower end of this range results in comparable muscle adaptations without the discomfort of the high pressures (5). It has been suggested that higher pressure (80% AOP) is needed for lower intensity exercise (10-20% 1RM) and the inverse relationship for higher intensity (40% 1RM) (8). In the research, cuff pressures range from 50 mmHg to 300 mmHg. It seems the best method is to calculate this with each person individually. Ideally the lowest pressure should be used that will still achieve the desired results.
Exercise Prescription
Low-load BFRT generally requires a higher volume of reps. It is generally prescribed as 75 repetitions within 4 sets. So this would look like 1 set of 30 reps, followed by 3 sets of 15 reps (30/15/15/15). 30 seconds rest is required between sets. Exercises are performed at 20-30% 1RM. The muscle group is trained 2-3 times per week. The reason for this high volume in a short period is metabolite accumulation which I will talk about below (6,10,12). See the tables below for a neat summary of parameters for both strength and aerobic exercise.
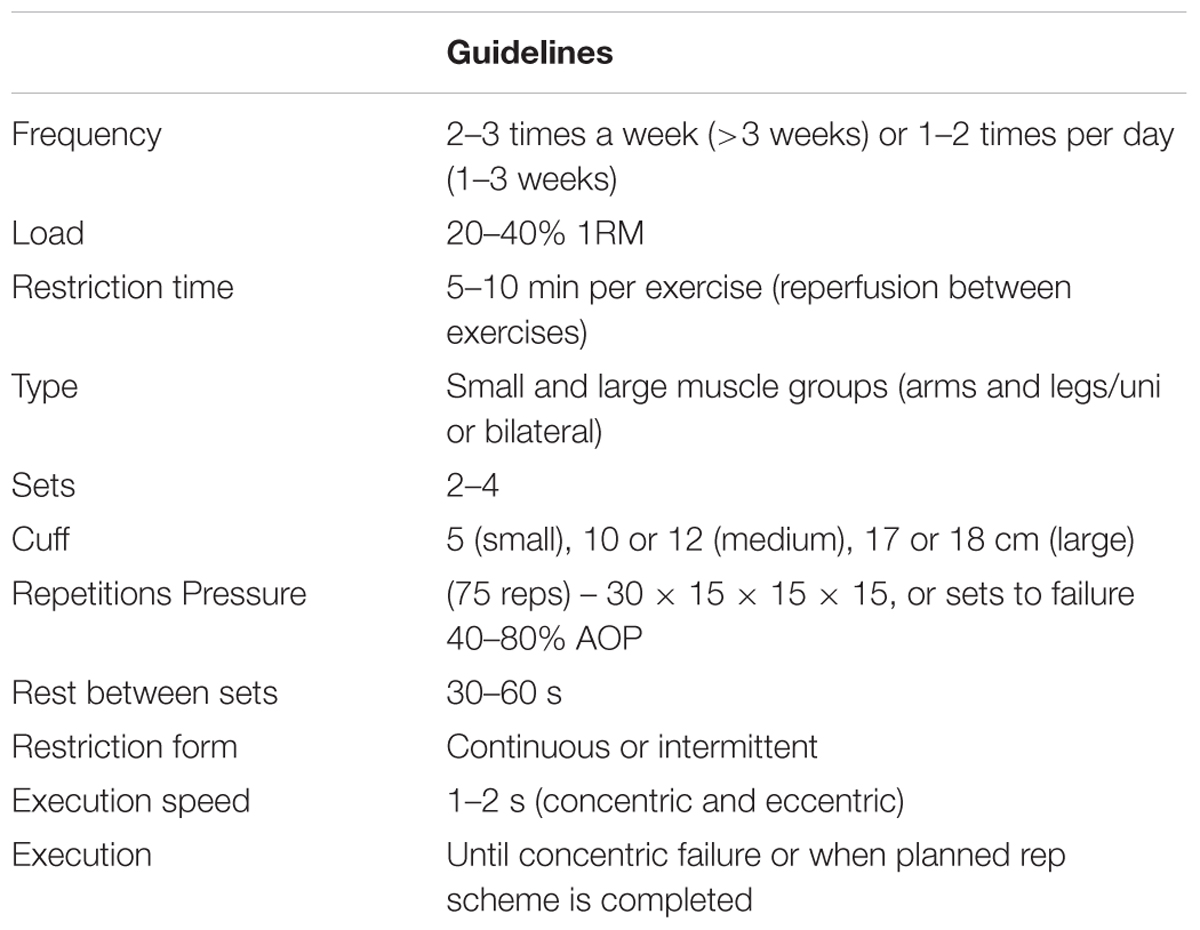
BFR strength training guidelines from Patterson et. al. 2019
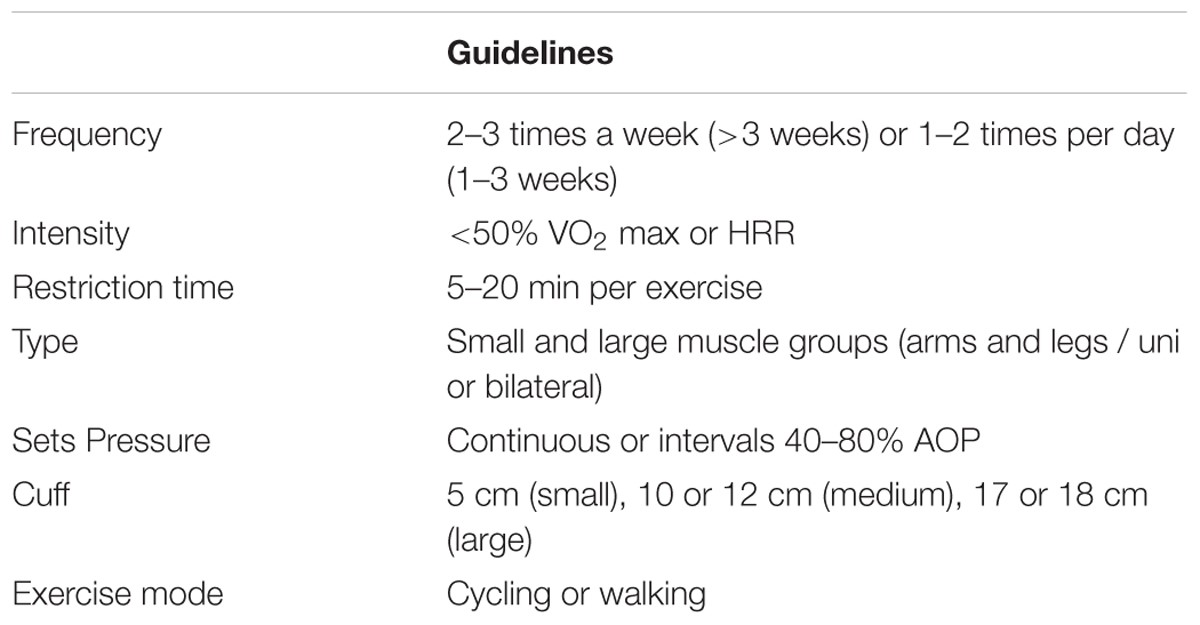
BFR aerobic exercise training guidelines from Patterson et. al. 2019
The science behind it
You might be thinking it sounds like some kind of fringe training technique but with a growing body of evidence BFRT has quickly become popularised. I won’t pretend I am a biologist but I will try to quickly summarise the scientific basis of BFRT.
For muscle growth, two things are required – mechanical tension on the muscles and metabolic stress. The restriction of blood flow causes metabolite accumulation (lactate, hydrogen ions) which can stimulate growth hormone and insulin-like growth factor-1 (IGF-1) which is a protein linked to muscle growth (12).
It has been shown that much like heavy resistance training, BFRT also decreases levels of myostatin which acts to control muscle remodelling (7). This is a good thing for building muscle. Cell swelling also occurs with the blood pooling from BFRT, this can stimulate myogenic stem cells and result in muscle hypertrophy.
In summary, we are yet to completely understand how BFRT works but the evidence shows that it does work.
Is it Safe?
There is not a great deal of evidence on the safety of BFRT. Concerns generally centre around the risk of venous thromboembolism (DVT / pulmonary embolism), muscle damage or the use of a tourniquet. Extreme muscle damage is called exertional rhabdomyolysis and the risk of this is extremely low (10). Risk of thromboembolism is likely mitigated with the use of clinical prediction rules and avoiding use of BFRT with higher risk subjects (2, 10). There is a low risk of tourniquet complications such as nerve and skin injury when using 3rd generation pneumatic, wide, and contoured tourniquet cuffs that reduce pressure levels (4).
Summary
- Blood flow restriction training allows similar hypertrophy and strength gains as heavy resistance training at lower loads
- Clinical populations can benefit from BFRT
- It appears to be safe as long as adequate care is taken
- Occlusion pressure needs to be 40-80% AOP
- High volume is used – approx. 75 reps over 4 sets with short rest periods
- The physiological basis of BFRT is not well understood although its effectiveness is supported in the current evidence
Resource
Listen here to The Physical Performance Show #149 to hear Mick Hughes discuss the use of BFRT in ACL Rehab

James Gardiner
POGO Physiotherapist
Book an Appointment with James here.
Featured in the Top 50 Physical Therapy Blog
References
- American College of Sports Medicine American College of Sports Medicine Position Stand. Progression models in resistance training for healthy adults. Med. Sci. Sports Exerc. 2009, 41, 687–708.
- Bond, C. W., Hackney, K. J., Brown, S. L., & Noonan, B. C. (2019). Blood flow restriction resistance exercise as a rehabilitation modality following orthopaedic surgery: A review of venous thromboembolism risk. Journal of Orthopaedic & Sports Physical Therapy, 49(1), 17-27.
- Centner, C., Wiegel, P., Gollhofer, A., & König, D. (2018). Effects of blood flow restriction training on muscular strength and hypertrophy in older individuals: A systematic review and meta-analysis. Sports Medicine, 49(1), 95-108.
- DePhillipo, N. N., Kennedy, M. I., Aman, Z. S., Bernhardson, A. S., O’Brien, L., & LaPrade, R. F. (2018). Blood flow restriction therapy after knee surgery: Indications, safety considerations, and postoperative protocol. Arthroscopy Techniques, 7(10), e1037-e1043.
- Hughes, L., Paton, B., Rosenblatt, B., Gissane, C., & Patterson, S. D. (2017). Blood flow restriction training in clinical musculoskeletal rehabilitation: A systematic review and meta-analysis. British Journal of Sports Medicine, 51(13), 1003-1011.
- Krzysztofik, Wilk, Wojdała, & Gołaś. (2019). Maximizing muscle hypertrophy: A systematic review of advanced resistance training techniques and methods. International Journal of Environmental Research and Public Health, 16(24), 4897.
- Laurentino, G. C., Ugrinowitsch, C., Roschel, H., Aoki, M. S., Soares, A. G., Neves, M., Aihara, A. Y., Da Rocha Correa Fernandes, A., & Tricoli, V. (2012). Strength Training With Blood Flow Restriction Diminishes Myostatin Gene Expression. Medicine & Science In Sports & Exercise, 44(3), 406-412.
- Lixandrão, M. E., Ugrinowitsch, C., Laurentino, G., Libardi, C. A., Aihara, A. Y., Cardoso, F. N., Tricoli, V., & Roschel, H. (2015). Effects of exercise intensity and occlusion pressure after 12 weeks of resistance training with blood-flow restriction. European Journal of Applied Physiology, 115(12), 2471-2480.
- Patterson, S. D., Hughes, L., Head, P., Warmington, S., & Brandner, C. (2017). Blood flow restriction training: A novel approach to augment clinical rehabilitation: how to do it. British Journal of Sports Medicine, 51(23), 1648-1649.
- Patterson, S. D., Hughes, L., Warmington, S., Burr, J., Scott, B. R., Owens, J., Abe, T., Nielsen, J. L., Libardi, C. A., Laurentino, G., Neto, G. R., Brandner, C., Martin-Hernandez, J., & Loenneke, J. (2019). Blood flow restriction exercise: Considerations of methodology, application, and safety. Frontiers in Physiology, 10.
- Tennent, D. J., Hylden, C. M., Johnson, A. E., Burns, T. C., Wilken, J. M., & Owens, J. G. (2017). Blood flow restriction training after knee arthroscopy. Clinical Journal of Sport Medicine, 27(3), 245-252.
- Vanwye, W. R., Weatherholt, A. M., & Mikesky, A. E. (2017). Blood Flow Restriction Training: Implementation into Clinical Practice. International Journal of Exercise Science.
- Yow, B. G., Tennent, D. J., Dowd, T. C., Loenneke, J. P., & Owens, J. G. (2018). Blood flow restriction training after Achilles tendon rupture. The Journal of Foot and Ankle Surgery, 57(3), 635-638.








