Knee Osteoarthritis
Definition, Cause and Prevalence
1 in every 10 people over the age of 50 are affected by knee osteoarthritis (OA) (3). Knee osteoarthritis is a complex peripheral joint disorder that results in reduced function with increased pain and stiffness (3) Knee OA is a degenerative condition that is a result cartilage breakdown from stress. Due to cartilages lack of blood supply, regeneration takes time, and with continued stress on the knee – the joint becomes inflamed, painful and stiff (2).
There are a large number of risk factors that predispose an individual to this disease (3). A history of diabetes, cancer, cardiovascular disease and walking disabilities are the main risk factors (2). Other factors such as age, gender (female), obesity, family history, trauma and malalignment also play a role (3). Knee OA is a chronic disease that is not localised as it affects the entire joint including its articular cartilage, meniscus, ligament and muscles (peri-articular) (2).
Knee OA is not only the most prevalent type of OA, it also presents at a younger age group compared to other OA types – particularly those who are obese (2).
Symptoms experienced from this condition, such as pain and stiffness have a profound effect on the individuals quality of life, both physically and psychologically (2).
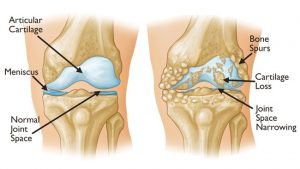
Diagnosis
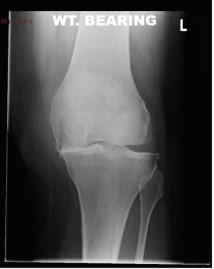
A diagnosis of knee OA is completed via a thorough history and clinical examination which is then confirmed by radiography (3). This is completed to rule out other sources that could be cause the reported knee pain (3).
Key features within the history of OA include persistent knee pain, limited morning stiffness and reduced overall function (2). Other reported symptoms include clicking of the knee (crepitus), reduced movement of the knee and any bony enlargement within the area (2).
On physical examination, tenderness may be felt over the involved joints, clicking may be heard when transitioning from sitting to standing, walking, or up/down stairs (2). It is also important to assess how the client walks (gait pattern) and measure both active and passive movements of the knee (2)(3).
Radiography remains the gold standard for diagnosing knee OA, however MRI has also been shown to be accurate (2)(3). The presence of osteophytes, joint space narrowing and malalignment are associated with knee OA, with osteophytes having the strongest relationship of the three (2)(3). However, many radiographic knee OA clients experience no symptoms, and in contrast, many clients with knee pain have no presence of knee OA on radiograph (2). Thus resulting in the need for a diagnosis that covers multiple assessment procedures.
Conservative Management of Knee Osteoarthritis
The disease’s slow progression allows a step-by-step approach to its management(3). When managing without the use of surgery, the focus areas are on client education, controlling pain and delaying the disease’s progression to improve function (3).
Lifestyle modification has been shown to be an effective approach to maintain function of the affected knee(s) (3). High-impact exercises such as running and jumping – particularly on hard surfaces – should be removed from the individual’s life and substituted for low-impact exercises such as swimming or cycling (3). Education and advise regarding weight loss, if the client was obese, has been shown to be effective as this is a large risk factor in developing or worsening knee OA (3).
Adding orthoses, improving footwear or using a knee brace are three methods to reduce client’s pain and improve function with knee OA (3). These items all improve the affected individual’s biomechanics and therefore reduce the load on the affected knee while also improving their perceived stability (3).

Physiotherapy that targets muscle strengthening and aerobic exercise has been supported by good quality evidence to provide benefit in the management of OA (3). Range-of-movement exercises to prevent contractures along with muscle strengthening of the quadriceps, hamstrings and calf muscles tend to stabilise the knee and improve the reported symptoms of the disease (3).
Physiotherapy that targets muscle strengthening and aerobic exercise has been supported by good quality evidence to provide benefit in the management of OA #physiowithafinishline @pogophysio Share on XNon-steroidal anti-inflammatory drugs (NSAIDs) are given to clients that experience a combination of a spike in both pain and inflammation of their knee(s) (3). These have been shown to reduce inflammation of the joint to both reduce pain and improve function (3).
Surgical Management
Party due to knee OA’s high prevalence, there are a number of operative methods to either preserve or replace the affected joint (3). These are summarised in table 1:
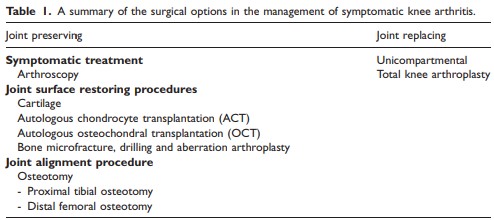
Arthroscopy is a common procedure aimed to trim (debride) the knee joint in an attempt to relieve the client’s symptoms (3). However, its use for OA is somewhat controversial (3) as research has shown that the symptomatic relief obtained from this procedure are a result of placebo (3). What has also been shown is that arthroscopies are most effective when the client experiences mechanical symptoms such as locking, joint tenderness, meniscal degenerative tear and mild to moderate presence of OA on radiograph imagery (3).
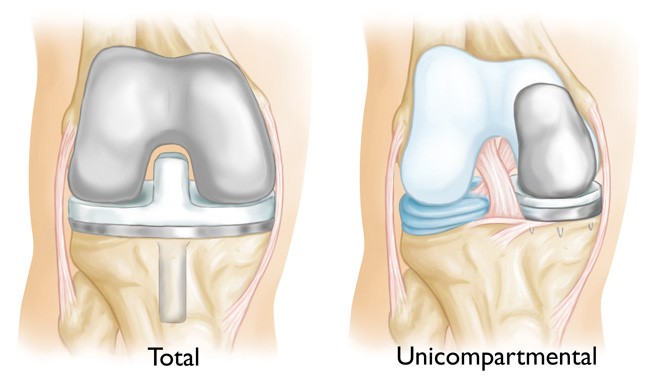
Unicompartmental knee arthroplasty (UKA) is a surgical intervention that replaces, due to the degenerative changes cause by OA, a part of the knee joint (1). Unlike the traditional total knee arthroplasty (TKA) or total knee replacement (1). Despite having benefits such as shorter surgical time, less blood loss, shorter rehabilitation and better knee range (3) – the UKA has shown a much higher revision and failure rate than the traditional TKA (1). This is due to a number of reasons such as bearing dislocations, mechanical loosening, replacement wearing, impingement or infection (1).
A more thorough, and more supported by research, approach is the total knee replacement (TKA). Advances in the design of the implants have resulted in better wear properties and more reproducible results (3). However, the timing of this intervention is still debated among researchers (3). The complication rate of the procedure is 5% of patients, this is due to infection (1.5%) or a blood clot in the legs or lungs (1-3%) (3). In conclusion, the total knee replacement (TKA) is the most effective and reliable surgical intervention, however, the client must be deemed appropriate through assessment and radiograph findings (3).
Conclusion
Knee Osteoarthritis affects a large number of individuals, and is the most common form of osteoarthritis (3). It is diagnosed through a series of history taking, physical assessment and imagery. Conservative (non-surgical) methods such as patient education, lifestyle adjustments, strengthening and mobility exercise prescription as well as appropriate medication such as anti-inflammatories should be pursued first (2)(3). Surgical intervention may be pursued if conservative methods fail. With multiple options available to clients, the correct procedure should be determined by a health professional that will return the client to their aspiring function as soon, and as safe, as possible.

Alec Lablache
POGO Physiotherapist
Featured in the Top 50 Physical Therapy Blog
References
- Campi, S., Tibrewal, S., Cuthbert, R., & Tibrewal, S. B. (2017;2018;). Unicompartmental knee replacement – current perspectives. Journal of Clinical Orthopaedics and Trauma, 9(2), 17-23. doi:10.1016/j.jcot.2017.11.013
- Heidari, B. (2011). Knee osteoarthritis prevalence, risk factors, pathogenesis and features: Part I. Caspian Journal of Internal Medicine, 2(3), 205.
- Hussain, S., Neilly, D., Baliga, S., Patil, S., & Meek, R. (2016). Knee osteoarthritis: A review of management options. Scottish Medical Journal, 61(2), 7-16. doi:10.1177/0036933015619588
- Umeda Con. (2018). Tricompartmental Osteoarthritis Knee. Retrieved from http://produtos-para-emagrecer.info/tricompartmental-osteoarthritis-knee.html\
- Trackactive.co. (2017). Exercises. Retrieved from https://app.trackactive.co/practices/1011/exercises