Diagnosis: Juvenile Arthritis
What is Juvenile Arthritis?
Juvenile Idiopathic Arthritis (JIA) is an inflammatory joint disease that lasts longer than 6 weeks in children and adolescents below the age of 16. It is a common arthritis that occurs in this population. It affects about 1 in 1,000 children every year, with 1 in 10,000 having a severe form of the disease.
It is not known what causes Juvenile Arthritis. It is an autoimmune disease, which means the body’s immune system attacks and destroys its own tissue for no apparent reason – particularly synovial membrane in moving joints. This breakdown of tissue causes inflammation which leads to joint pain, swelling and stiffness. It is believed that changes in the environment and mutations of certain viruses can trigger JIA.
Juvenile Arthritis is an autoimmune disease, which means the body’s immune system attacks and destroys its own tissue #performbetter @pogophysio Share on XHow Juvenile Arthritis Presents
Children with JIA will present with symptoms that are generally characteristic of arthritis – i.e. joint pain, swelling and stiffness, especially when getting up in the mornings or after a nap. Loss of joint range of motion can develop and lead to suboptimal compensatory movements such as limping.
There are 3 main subtypes of JIA: Oligoarticular; Polyarticular and Systemic.
Oligoarticular is the most common, accounting for 50% – 60% of JIA cases. Girls are more susceptible than boys. It affects up to 4 joints (oligo meaning few), and usually they are the large joints of the body (the ankles, knees, wrists and elbows) and mainly only affects one side of the body. It is generally the mildest form of the disease, and permanent damage is rare. However, if uveitis (eye inflammation) develops, they need to be closely monitored by an ophthalmologist.
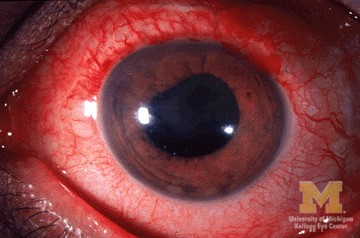
Uveitis (author: Jonathan Trobe; source: WikiMedia Commons)
Polyarticular affects about 40% of children with JIA and also more common in girls than boys. It affects 5 or more joints, usually smaller joints of the hands and feet on both sides of the body. The hips can also be affected. Children with positive Rheumatoid Factor between ages 9 and 16 have a poor prognosis, with 50% progressing to severe disabling arthritis in adulthood. Other symptoms associated with this form of JIA are fatigue, a poor appetite, weight loss, low fever and general feeling of being unwell.
Systemic-onset JIA (SoJIA), or Still’s Disease accounts for 10 – 20%, with males and females affected equally, often in early childhood. This is the most severe type. As well as joint pain, children also experience repeating fevers, skin rash, fatigue, widespread aches and pains and also inflammation and swelling of internal organs such as the heart, liver, spleen and lymph nodes. About a half of children with SoJIA will fully recover.
How Juvenile Arthritis is Diagnosed
Juvenile Arthritis is mostly diagnosed via medical examinations prescribed by your doctor. Generally, diagnosis is difficult because the symptoms are similar to other diseases. No single test can confirm JIA, but doctors will usually rely on the clinical presentation, blood tests and X-Rays to make an initial diagnosis.
Treatment of Juvenile Arthritis
The goal of physiotherapy is to help the child return to normal levels of physical and social activities. While JIA will inevitably limit the child’s ability to participating in certain physical activities, they should be encouraged to remain as active as possible, especially during periods of remission (when the condition settles down). Regular activity can reduce the severity of the symptoms.
Physiotherapy focuses on maintaining muscle tone and relaxation, strength, range of motion, joint protection.
During periods of flare-ups, rest and pain reducing therapies should be applied. These include ultrasound, hydrotherapy, heat and cold packs and paraffin wax dips.
Wayne Wu
Student Physiotherapist
References
(Betz, Lonnemann, & Walker, n.d.; Cellucci et al., 2009a; Wikipedia contributors, 2016) (Cellucci et al., 2009b; Schneider & Queffelec, 2016)
Betz, E., Lonnemann, E., & Walker, W. (n.d.). Juvenile Rheumatoid Arthritis Retrieved December 06, 2016, from http://www.physio-pedia.com/Juvenile_Rheumatoid_Arthritis
Cellucci, T., Huber, A., Levin, A. V., McGrath, P. J., Schanberg, L. E., Spiegel, L., . . . Tucker, L. B. (2009a, December 20, 2009). Juvenile Idiopathic Arthritis – Oligoarticular Arthritis Retrieved December 06, 2016, from http://www.aboutkidshealth.ca/En/ResourceCentres/JuvenileIdiopathicArthritis/AboutJIA/TypesofJIAinChildrenandTeenagers/Pages/OligoarticularArthritis.aspx
Cellucci, T., Huber, A., Levin, A. V., McGrath, P. J., Schanberg, L. E., Spiegel, L., . . . Tucker, L. B. (2009b, December 20, 2009). Juvenile Idiopathic Arthritis – Polyarticular Arthritis Retrieved December 06, 2016, from http://www.aboutkidshealth.ca/En/ResourceCentres/JuvenileIdiopathicArthritis/AboutJIA/TypesofJIAinChildrenandTeenagers/Pages/OligoarticularArthritis.aspx
Schneider, R., & Queffelec, K. (2016, January 11, 2016). Systemic Juvenile Idiopathic Arthritis (sJIA) Retrieved December 06, 2016, from http://www.aboutkidshealth.ca/En/HealthAZ/ConditionsandDiseases/InflammatoryConditions/Pages/Systemic-Juvenile-Idiopathic-Arthritis-SJIA.aspx
Wikipedia contributors. (2016, October 17, 2016). Juvenile idiopathic arthritis Retrieved December 06, 2017, from https://en.wikipedia.org/w/index.php?title=Juvenile_idiopathic_arthritis&oldid=744754371








