Exercise: why do Physio’s prescribe it?

If you’ve ever had physiotherapy treatment you likely will have walked away from your consultation with some ‘homework’ in the form of prescribed exercises. Depending on your experience with such exercises you’ll likely have formed an opinion on this. Maybe you love them, maybe you find them torture but commit to the process and see results, or maybe you’re the person who smiles, nods and hopes their physio stops asking about whether they have completed said exercises. Regardless which bucket you fall into, your physio has prescribed these movements to create a specific effect, which is what I aim to explore through this blog.
What is exercise?
Initially, it is helpful to define what is exercise and what it isn’t. Exercise is “planned, structured, and repetitive movement and has as a final or an intermediate objective the improvement or maintenance of physical fitness”. This is different to physical activity which is defined as “any bodily movement produced by skeletal muscles that results in energy expenditure” (2). Exercise is movement completed with a health purpose. Exercise can come in the form of aerobic, resistance, flexibility, balance.
Why do we use it?
Exercise Induced Hypoalgesia
Exercise Induced Hypoalgesia (EIH) is a reduction in pain and pain sensitivity during and after exercise occurs. This is reasonably reliably occurring in healthy, pain-free individual however can be less predictable in the persistent pain populations (the mechanism is sometimes impaired). Many studies have experimentally found that aerobic exercise, dynamic resistance and isometric resistance exercise are effective at reducing measures of pain sensitivity. However aerobic exercise appears to have the largest effect on pain reduction (9,10). Quite simply, exercise can be a natural pain reliever.
Less is known about exactly what dose of exercise is most effective for pain reduction. A large study was published in 2019 which was unable to provide a clear answer for the frequency, time or duration of exercise needed for analgesia (8).
Whilst we know pain can improve through exercise, in persistent pain exercise may be less effective or actually increase pain. This variable response may be a deterrent to exercise for this population however this EIH mechanism is not impaired in all persistent pain patients and exercise has definitely been shown to be effective. A 2017 Cochrane Review found that for persistent (chronic) pain, exercise had variable effects on pain severity, exercise improved physical function a small-moderate amount, either improved or had no effect on psychological function and quality of life and there was low risk of any adverse event (4).
Tissue Capacity
Let me explain the process of “mechanotransduction”. This is the natural process where the body converts mechanical stimulus into cellular responses. This occurs in three general steps;
- Mechanocoupling – this is the mechanical trigger or stimulus.
- Cell-cell communication – cells talk to each other and the signal is passed through the tissue.
- Effector cell response – this is the cellular response for increased production of that tissue. (6)
Our bodies are highly adaptable and when we place loads that are higher than the normal, the tissue adapts and becomes larger and stronger. As long as they’re not so far above the tissues capacity that they cause injury. And this line is what we aim to navigate in rehabilitating injuries, where the goal is tissue repair and remodelling. The larger the tissue’s capacity, the more load it can withstand.

Image: the balancing act of loading versus tissue capacity
General Health
Another key reason for exercise prescription is to combat chronic diseases huge burden on society. Routine physical activity has continually been shown to reduce risk of premature mortality and be an effective preventor of over 25 chronic diseases (11). As health professionals and physical therapists, the encouragement of appropriate exercise and physical activity is essential.
Does a physical job count as exercise? … The ‘physical activity paradox’
Remember those definitions about the difference between exercise and physical activity? Exercise is intended to improve health, work is not. And yes, work is important (for social, psychological, economical, physical reasons) and yes you do expend energy, use muscles, lift heavy things etc. etc. but it doesn’t not have the same effect on your health as exercise (5).
The issues with work related physical activity are:
- too low intensity – often completed at 30-35% max. aerobic capacity where 60-70% is required for improving fitness.
- too prolonged – think an 8 hour work day versus 30-60 minute training session.
- not enough recovery time – work is completed 7-12 hours per day for consecutive days. If an athlete trained this way it would be considered overtraining.
- prolonged static posturing & heavy lifting – can lead to sustained elevated blood pressure.
- worker has too little control over the activity – exercise is generally performed when the person wants to, for how long they desire, in a safe environment of their choice. Often workers have limited control of the environment, hours, and stressors.
A study published in 2018 even found that really high levels of occupational physical activity could be detrimental and cause increase risk of earlier mortality (3).
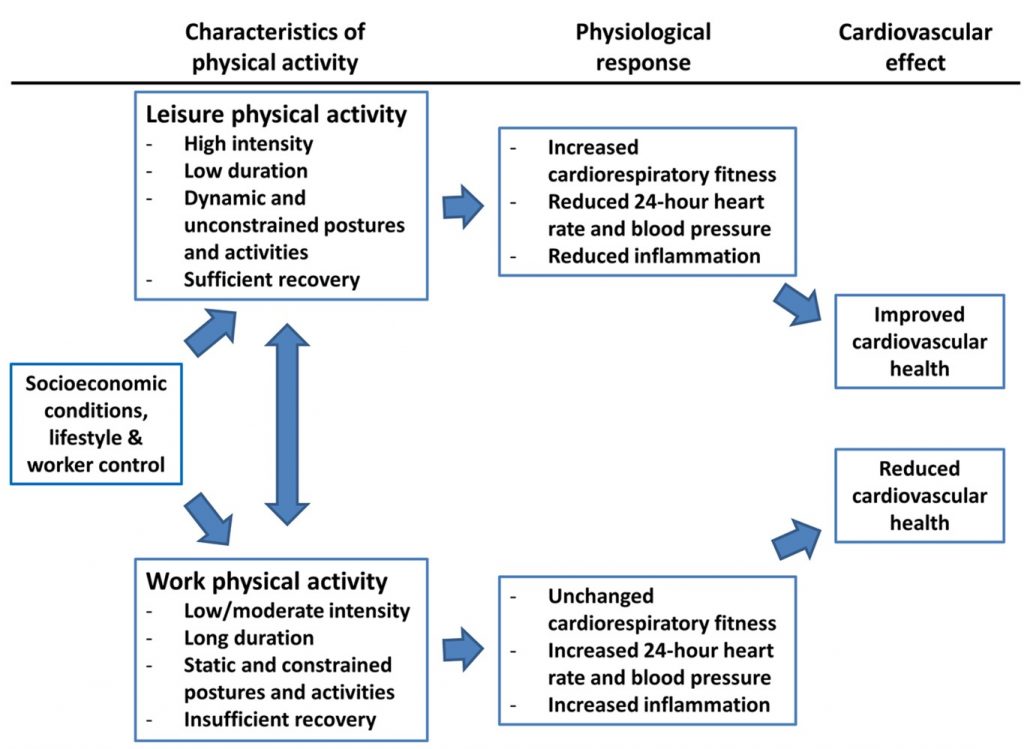
Image: Conceptual diagram of the proposed mechanisms behind the physical activity health paradox (Holtermann, 2017).
Conclusion
Exercise is not a panacea, it isn’t the saviour or solution to all the worlds health problems. But in world where over 72% of deaths occur from non-communicable chronic diseases, I see very little down side or adverse effects when exercise prescribed appropriately as a treatment. Exercise has many scientifically documented benefits (1), it is very low cost and often works as well as medications for treatment of disease (7).
In terms of rehabilitation of injuries, manipulating mechanotransduction to improve tissue capacity and the possibility for exercise induced analgesic effects are key reasons for the that little bit of homework you have been given.

James Gardiner
Physiotherapist
Book an Appointment with James here.
Featured in the Top 50 Physical Therapy Blog
References
- Anderson, E., & Durstine, J. L. (2019). Physical activity, exercise, and chronic diseases: A brief review. Sports Medicine and Health Science, 1(1), 3-10.
- Caspersen, C. J., Powell, K. E., & Christenson, G. M. (1985). Physical activity, exercise, and physical fitness: definitions and distinctions for health-related research. Public Health Reports, 100(2), 126-131.
- Coenen, P., Huysmans, M. A., Holtermann, A., Krause, N., Van Mechelen, W., Straker, L. M., & Van der Beek, A. J. (2018). Do highly physically active workers die early? A systematic review with meta-analysis of data from 193 696 participants. British Journal of Sports Medicine, 52(20), 1320-1326.
- Geneen, L. J., Moore, R. A., Clarke, C., Martin, D., Colvin, L. A., & Smith, B. H. (2017). Physical activity and exercise for chronic pain in adults: An overview of Cochrane reviews. Cochrane Database of Systematic Reviews.
- Holtermann, A., Krause, N., Van der Beek, A. J., & Straker, L. (2017). The physical activity paradox: Six reasons why occupational physical activity (OPA) does not confer the cardiovascular health benefits that leisure time physical activity does. British Journal of Sports Medicine, 52(3), 149-150.
- Khan, K. M., & Scott, A. (2009). Mechanotherapy: How physical therapists’ prescription of exercise promotes tissue repair. British Journal of Sports Medicine, 43(4), 247-252.
- Naci, H., & Ioannidis, J. P. (2013). Comparative effectiveness of exercise and drug interventions on mortality outcomes: Metaepidemiological study. BMJ, 347(oct01 1), f5577-f5577.
- Polaski, A. M., Phelps, A. L., Kostek, M. C., Szucs, K. A., & Kolber, B. J. (2019). Exercise-induced hypoalgesia: A meta-analysis of exercise dosing for the treatment of chronic pain. PLOS ONE, 14(1), e0210418.
- Rice, D., Nijs, J., Kosek, E., Wideman, T., Hasenbring, M. I., Koltyn, K., Graven-Nielsen, T., & Polli, A. (2019). Exercise-induced Hypoalgesia in pain-free and chronic pain populations: State of the art and future directions. The Journal of Pain, 20(11), 1249-1266.
- Wewege, M. A., & Jones, M. D. (2020). Exercise-induced Hypoalgesia in healthy individuals and people with chronic musculoskeletal pain: A systematic review and meta-analysis. The Journal of Pain.
- Warburton, D. E., & Bredin, S. S. (2017). Health benefits of physical activity: a systematic review of current systematic reviews. Current Opinion in Cardiology, 32(5), 541-556.








